Combined oral contraceptive pill
The combined oral contraceptive pill (COCP) is a contraceptive for women. It is often called birth control pill or simply "the pill." The pills contain hormones that make the women who take them infertile. Women who take the pill will not become pregnant during sexual intercourse. When a woman stops taking the pills, she will usually become fertile again. When taken as prescribed, the pills are one of the safest methods of contraception.
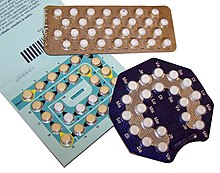
In the 1950s, scientists (such as Carl Djerassi, George Rosenkranz and Alejandro Zaffaroni) realized that the hormone progesterone stopped women from making eggs (stopped ovulation). After this discovery, the combined oral contraceptive pill was created.[1] The combined oral contraceptive pill has two female hormones: estrogen and progesterone. Some oral contraceptive pills have only progesterone. These are often called the "minipill".
The combined oral contraceptive pill is thought to be safe and usually works well.[2]
In the United States, the combined oral contraceptive pill was first given to women in 1960.[3] It was a revolutionary breakthrough in contraception for two reasons. First, it is very effective at preventing pregnancy if it is used in the right way. Second, it was the first contraceptive to completely separate the act of contraception (in this case the taking of a pill) from sexual intercourse itself. Unlike barrier methods, when a woman is "on the Pill," she and the man are usually not even aware of it during sexual intercourse, which seems and feels very natural. The woman may be on the pill without her partner knowing. The couple can have sex at any time they wish; they don’t need to interrupt foreplay to put birth control in place, and they can feel the physical sensations and emotional closeness of intercourse without interference from a male or female condom. Unlike coitus interruptus, when a woman is on the Pill, intercourse usually ends with her man reaching orgasm while inside the vagina, which both the man and woman usually find very pleasurable. It may also make women's menses shorter and with less bleeding, as well as helping her complexion, which most women like. For all of these reasons, the Pill is very popular. In 2005, more than 80 million women across the world used the Pill.[4] It is the most common method of contraception in the United States, with four out of five women there having used the pill for birth control at some point in their lives.[5] Use of the Pill is different in different countries,[4] and among women of different ages and levels of education.[6] Both single women and married women use the Pill in large numbers.
The Pill has some slight risks for side effects. It may make a very small increase in the risk of blood clots in the lungs, strokes, heart attacks, and breast cancer. Most of these risk are small. Some women may experience mood swings, weight gain, or loss of sex drive. Sometimes these side effects are serious enough to make a woman decide to stop using the Pill.
Different countries use different contraceptives
changeThe choices a woman has for contraception - and whether contraception is even available - depends on what country she lives in. These things are different in different countries. In the United Kingdom, one out of every 4 women aged 16–49 were using the Pill as at 2006 (either the combined pill or progestogen only pill ("minipill")).[7] compared to only 1% of women in Japan.[8] Local culture and habits affect whether or not people use the Pill.[9][10]
In some countries, women do not really have a choice because only one kind of contraception is available.[11] In some countries (like Algeria, Morocco, and Zimbabwe), the Pill is the most common method offered by national family planning programs. In other countries, like India, national family planning programs only offer female sterilization (a surgery which makes a woman unable to ever have children again). Other countries, like Egypt and Vietnam, only offer the IUD, intrauterine device.[4][11]
Different kinds of pills
changeThere are two major kinds of oral contraceptive pills. The first kind has both estrogen and progesterone in it. The other only has progesterone (these are called progesterone-only pills, or POPs). The pills do not actually have natural hormones in them. Instead, they have other chemical substances that are mostly the same as the hormones, but have been made in a laboratory.
Some women can only take one kind of COCP. For example, estrogen stops the breast from producing milk. Because of this, women who are breastfeeding should not take pills that have estrogen in them. There are also some other types of women who should not be given estrogen. These women should only use progesterone-only pills.
While there are just two major kinds of birth control pills (COCPs and POPs), there are many different brands or versions of each kind of pill. Every brand of COCP will have the same hormones (estrogen and progesterone) in it. However, each brand has a different amount of hormones in it. Also, some brands change the amount of hormones given from week to week.
Effectiveness
changeThere are two ways to measure how well COCPs work. (Most forms of birth control are also measured in these two ways.):
- We can look at how well the Pill works in cases of perfect use. This means that the Pill has been used exactly how it is supposed to be used. The women using the Pill are assumed to have made no mistakes in how they used it. (For example, they have taken every dose on time, without missing any doses.)
- We can look at how well the Pill works in cases of actual use or typical use. It is not realistic to think that every woman uses the Pill perfectly. Some women use the pill the wrong way, miss doses, or stop taking the pill. This makes the Pill's effectiveness (how often it prevents pregnancy) lower.
To show how well the Pill works, scientists figure out rates of effectiveness (for perfect use and for actual/typical use). These rates show how many women are kept from getting pregnant by the Pill. Rates of effectiveness usually look at how well the Pill works during the first year that women are using the Pill.[12] Most often, the Pearl Index is used to calculate effectiveness rates. However, some studies use decrement tables.[13]
The typical use pregnancy rate for women taking COCPs measures how many women get pregnant while taking them. All women are not equally likely to get pregnant while taking COCPs. Different groups of women have different typical pregnancy rates. Overall, between 2% and 8% of women taking COCPs get pregnant every year. If they are used perfectly only 0.3% become pregnant each year.[12]
There are a few reasons why women do not use the Pill perfectly. Because of these things, typical use effectiveness is lower than perfect use effectiveness.
- People are not always told how to use the Pill correctly. (For example, they are not given the right information about how often the Pill should be taken.)
- People sometimes make mistakes without knowing what they have done wrong. (For example, a woman might forget to take the Pill.)
- People sometimes make mistakes on purpose. A woman might not get new pills from the pharmacy. She might also decide to stop taking the Pill, or skip doses, if she decides she wants to get pregnant.[14]
COCPs can prevent pregnancy if the first pill is taken no later than 5 days after a woman starts menstruating. If the treatment is started at any other time in the menstrual cycle, COCPs cannot safely prevent pregnancy for the first 7 days of use. During this time, a woman needs to use other types of contraception in order to prevent pregnancy. When active pills have been taken for 7 days, they can work well to prevent pregnancy. They should be taken at about the same time every day.[15][16]
Certain things can make COCPs not work as well:
- If a woman misses more than one active pill in a packet. (Certain packets also contain "placebo pills", which do not have any hormones in them. COCPs are usually used for three weeks out of the month. The woman then takes a break from the pills for a week. Some packets have placebo pills for women to take during this week, so that the woman does not get out of the habit of taking a pill every day. If a woman does not take placebo pills during this week, it does not make her more likely to get pregnant.)
- If a woman waits more than a week to start taking COCPs (active pills) again, after her week-long break.
- If a woman's body has problems with absorbing active pills (for example, if the woman has diarrhea or vomiting).
- If a woman is taking other medicines which interact with her COCPs to make them not work as well (for example, medicines which lower her estrogen or progestogen levels).[15]
Problems with other drugs
changeSome other medicines can interact with COCPs and make them not work as well. These medicines can also cause breakthrough bleeding (where a woman bleeds between her periods). Some of these medicines are:
- Some antibiotics which are used to treat tuberculosis and meningitis (like rifampicin)
- Some sedatives (especially barbiturates)
- Some drugs to treat epilepsy (like phenytoin and carbamazepine)
- Broad-spectrum antibiotics, like ampicillin and doxycycline. These medicines may cause problems "by impairing the bacterial flora responsible for recycling ethinylestradiol from the large bowel" (BNF 2003). This means that a person's large intestine does not take up estradiol the way it should.[17]
The traditional medicinal herb St. John's Wort also seems to make COCPs not work as well. This is because of the way St. John's Wort affects the liver.
Non-contraceptive uses
changeThe Pill can be used for other things besides contraception. There are many medical conditions that are caused by problems with hormone levels. Because the Pill has hormones in it, it can treat these conditions. Some of these conditions are:
- Anemia caused by menstruation
- Painful menstruation (dysmenorrhea)
- Mild or moderate acne.[18]
If a woman's menstrual cycle is not regular, the Pill can make the woman menstruate on a regular schedule. The Pill can also be used to treat certain problems that cause bleeding from the uterus.
Women who use combined oral contraceptives are less likely to get cancer of the ovaries. If a woman takes Pill for five years, her risk for getting ovarian cancer is cut in half. Women taking the Pill are also only half as likely to get endometrial cancer than women who have never taken the Pill. The longer a woman uses the Pill, the more her risk of getting endometrial cancer drops. However, women who take the Pill have a higher risk of getting breast cancer and cervical cancer.[19]
References
change- ↑ Baird, David T.; Anna F. Glasier (May 27, 1993). "Hormonal Contraception". Volume 328:1543-1549 May 27, 1993 Number 21 Review Article - Drug Therapy. 328 (21). New England Journal of Medicine: 1543–1549. doi:10.1056/NEJM199305273282108. PMID 8479492. Archived from the original on October 28, 2006. Retrieved 2008-11-17.
- ↑ Schwartz, Jill L.; Henry L. Gabelnick (2002). "Current Contraceptive Research" (PDF). Vol. 34, No. 6 (November/December 2002), Pp. 310-316. 34 (6). Perspectives on Sexual and Reproductive Health: 310–316. PMID 12558094. Retrieved 2008-11-17.
- ↑ Goldin, Claudia; Lawrence F. Katz (2002). "The Power of the Pill: Oral Contraceptives and Women's Career and Marriage Decisions" (abstract). Journal of Political Economy, 2002, Vol. 110, No. 4. 110 (4). University of Chicago: 730–770. doi:10.1086/340778. S2CID 221286686.
- ↑ 4.0 4.1 4.2 UN Population Division (2006). World Contraceptive Use 2005 (PDF). New York: United Nations. ISBN 92-1-151418-5. In 2005, there were 1,097,427,000 women in the world between the ages of 15-49, who were married or in union (living with a partner in a marriage-like relationship). Of these women, 7.5% used the Pill. However, in different countries, there are a lot of differences in how many women use the Pill. For example, in the United States, 15.6% of women in relationships use the Pill. In the United Kingdom, 22% do. In Japan, the Pill is much less common; only 2.3% of women in relationships use either the Pill or anIUD as well. The numbers for some other countries are: Algeria, 44.3%; Morocco, 40.1%; Zimbabwe, 35.5%; India, 2.1%; Egypt, 9.3%; Vietnam, 6.3%.
- ↑ Mosher WD; Martinez GM; Chandra A; Abma JC; Willson SJ (2004). "Use of contraception and use of family planning services in the United States: 1982-2002" (PDF). Adv Data (350): 1–36. PMID 15633582.
The leading method of contraception in the United States in 2002 was the oral contraceptive pill. It was being used by 11.6 million women 15–44 years of age; it had ever been used by 44.5 million women 15–44 years of age.
- ↑ S Hamid and R Stephenson (2006). "Provider and Health Facility Influences On Contraceptive Adoption in Urban Pakistan" (PDF). International Family Planning Perspectives. 32 (2): 71–78. doi:10.1363/3207106. PMID 16837387.
- ↑ Taylor, Tamara; Keyse, Laura; Bryant, Aimee (2006). Contraception and Sexual Health, 2005/06 (PDF). London: Office for National Statistics. ISBN 1-85774-638-4. Archived from the original (PDF) on 2007-01-09. British women aged 16-49: 24% currently use the Pill (17% use Combined pill, 5% use Minipill, 2% do not know type)
- ↑ Aiko Hayashi (2004-08-20). "Japanese Women Shun The Pill". CBS News. Archived from the original on 2006-06-29. Retrieved 2006-06-12.
- ↑ AV Camacho and MD Castro and R Kaufman (2006). "Cultural aspects related to the health of Andean Women in Latin America: A key issue for the attainment of progress towards the Millenium Development Goals" (PDF). International Journal of Gynecology and Obstetrics (94): 357–363. Archived from the original (PDF) on 2007-07-05. Retrieved 2008-11-18.
- ↑ A Srikanthan and RL Reid (2008). "Religious and Cultural Influences on Contraception" (PDF). J Obstet Gynaecol Can. 30 (2): 129–137. doi:10.1016/S1701-2163(16)32736-0. PMID 18254994. Archived from the original (PDF) on 2010-06-20. Retrieved 2008-11-18.
- ↑ 11.0 11.1 Bongaarts, John; Elof Johansson (2000). "Future Trends in Contraception in the Developing World: Prevalence and Method Mix" (PDF). Revised version of a paper prepared for the IUSSP Seminar on “Family Planning Programmes in the 21st Century” at ICDDR,B, Dhaka, January 2000. The Population Council (international, nonprofit, nongovernmental organization). Archived from the original (PDF) on 2008-11-17. Retrieved 2008-11-17.
- ↑ 12.0 12.1 Hatcher, RA; Trussel J, Stewart F; et al. (2000). Contraceptive Technology (18th ed.). New York: Ardent Media. ISBN 0-9664902-6-6. Archived from the original on 2008-05-31. Retrieved 2008-11-17.
- ↑ Kippley, John; Sheila Kippley (1996). The Art of Natural Family Planning (4th ed.). Cincinnati, OH: The Couple to Couple League. pp. 141. ISBN 0-926412-13-2.
- ↑ They want to get pregnant, put their partner does not want them to
- ↑ 15.0 15.1 Speroff, Leon; Darney, Philip D. (2005). "Oral Contraception". A Clinical Guide for Contraception (4th ed.). Philadelphia: Lippincott Williams & Wilkins. pp. 21–138. ISBN 0-7817-6488-2.
- ↑ FFPRHC (2007). "Clinical Guidance: First Prescription of Combined Oral Contraception" (PDF). Archived from the original (PDF) on 2007-07-04. Retrieved 2007-06-26.
- ↑ The effects of broad-spectrum antibiotics on Combined contraceptive pills is not found on systematic interaction metanalysis (Archer, 2002), although "individual patients do show large decreases in the plasma concentrations of ethinylestradiol when they take certain other antibiotics" (Dickinson, 2001). "...experts on this topic still recommend informing oral contraceptive users of the potential for a rare interaction" (DeRossi, 2002) and this remains current (2006) UK Family Planning Association advice Archived 2007-02-08 at the Wayback Machine.
- Archer J, Archer D (2002). "Oral contraceptive efficacy and antibiotic interaction: a myth debunked". J Am Acad Dermatol. 46 (6): 917–23. doi:10.1067/mjd.2002.120448. PMID 12063491.
- Dickinson B; Altman R; Nielsen N; Sterling M (2001). "Drug interactions between oral contraceptives and antibiotics". Obstet Gynecol. 98 (5 Pt 1): 853–60. doi:10.1016/S0029-7844(01)01532-0. PMID 11704183. S2CID 41354899.
- DeRossi S, Hersh E (2002). "Antibiotics and oral contraceptives". Dent Clin North Am. 46 (4): 653–64. doi:10.1016/S0011-8532(02)00017-4. PMID 12436822.
- ↑ Huber J, Walch K (2006). "Treating acne with oral contraceptives: use of lower doses". Contraception. 73 (1): 23–9. doi:10.1016/j.contraception.2005.07.010. PMID 16371290.
- ↑ "Oral Contraceptives and Cancer Risk: Questions and Answers". National Cancer Institute Fact Sheet. National Cancer Institute (US Government). Retrieved 2008-11-27.